Author: Julia Hart
Posted March 2026
Introduction
Recent work has established psychedelic-assisted therapy (PAT) as an impactful form of healing for PTSD, depression, anxiety, and existential suffering in people diagnosed with cancer (Schipper et al., 2024). In the context of clinical trials, these psychedelic experiences are facilitated by a trained therapist, who acts both as an empathetic presence and follower of the participant. The presence of a therapist is foundational to the mediated psychedelic experience of the participant, although models through which PAT is conducted are still in early stages of development. A variety of different psychotherapeutic models have been utilized in the clinical trials of psychedelic compounds, varying from early psycholytic treatment (including multiple and very involved talk-therapy sessions) to the more recent, psychedelic therapy, (non-directive therapeutic approaches, in conjunction with preparation and integration sessions) (Garcia-Romeu & Richards, 2018). Building upon this work, this blog explores the concept of interpersonal grounding by discussing key relational elements, defining the beginnings of a framework to foster quality connection between therapist and participant in the PAT healing context.
Definitions
Psychedelic-assisted therapy (PAT) is a form of integrational psychotherapy that combines the power of consciousness-altering substances with a trained therapist (Association for Behavioral and Cognitive Therapies, 2023). Increasingly, studies show that PAT has the potential to improve symptoms of depression, anxiety, and PTSD in patients experiencing psychological distress (Grob et al., 2011). PAT also has potential to reduce end-of-life existential dread for those with life-limiting cancer diagnoses (Griffiths et al., 2016; Richards et al., 1977).
Interpersonal grounding refers to the therapeutic alliances cultivated between participants and therapists during PAT. A foundational book on the topic defines interpersonal grounding as “the quality of the human relationship that enables the person who has received the psychedelic to feel safe, open, curious, and courageous as the opportunities to explore the human mind opens up” (Richards, 2015). Interpersonal grounding comprises the techniques employed within the therapist-participant relationship that foster relational validation and comfort throughout the PAT journey. The concept of interpersonal grounding has been cultivated and conceptualized largely by Bill Richards, a pioneering psychotherapist in the field of PAT. Little empirical study has been conducted surrounding how interpersonal grounding manifests in practice. In anticipation of the growing demand and need to scale PAT, the identification of therapeutic techniques and dynamics used between therapists and participants is critical (Phelps, 2017).
Historical Context
In attempting to define, categorize, and apply the elements employed in modern clinical practice it is important to acknowledge that psychological and somatic healing with psychotropic compounds has been practiced, revered, and deeply understood by indigenous people for millennia. In observing instances of indigenous psychoactive healing practices and interpersonal dynamics between healer and participant, the Western world is among the last of global cultures and societies to involve itself in this practice (Falcon, 2025).
Seemingly innumerable groups have used psychoactive plants in ritualistic and medicinal settings, especially in instances of indigenous shamanistic figures utilizing psychotropic compounds to heal their communities (Schenberg, 2022). Psychoactive compounds, such as those included in the Psilocybe genus, are widely available in native plants on every continent save Antarctica (Rodriguez, 2021). The characteristics, practices, and attitude of a psychotherapist may be seen as sharing many qualities with that of an effective healing shaman (McKenna, 1990). This is not to say we must implement and mimic actions of shamanism in the modern practice of PAT, but we should recognize the similarities between traditional and Western interpretations and usages of PAT, and approach this field with humility and respect rather than purely with novelty.
Data
In order to identify and categorize moments of interpersonal grounding, I analyzed data derived from an open-label, Phase 2 clinical trial that examined the efficacy of group psilocybin-assisted therapy for treating major depressive disorder in people living with cancer and depression (Agrawal et al., 2024). These trials within the study consisted of two preparation sessions, the dosing day, and two integration sessions to reflect and internalize insights drawn from the PAT experience. I focused on interpersonal grounding moments occurring during dosing days, during which participants received capsules containing 25mg of synthetic psilocybin. Across the entirety of the sessions, a therapist certified in PAT was present to offer grounding to the participant through the duration of their treatment. An additional therapist monitored the session on-site in real time by video to assist if the need arose.
Methods
Previous work in the Vermont Conversation Lab (Gramling et al., 2023), identified instances of human connection moments in PAT (defined by inclusion of proposed best-practice competencies, i.e., empathic abiding presence and interpersonal grounding). In this study, three investigators each coded four dosing day videos (each approx. 8 hours) and found 372 moments of therapeutic connection. This previous study defined interpersonal grounding as being a definitional part of human connection within PAT.
My investigation of interpersonal grounding in this study took these coded moments of human connection as a starting point. When one or more of the three coders for each video marked a moment of human connection, I analyzed it as a potential interpersonal grounding moment. Through this process, I identified moments of interpersonal grounding, creating a matrix to organize recurrent patterns, as well as illustrative quotes. Once all 4 videos were coded, I categorized key elements within identified themes in moments of interpersonal grounding. I maintained rigor throughout this process by memoing alongside the coding process, and debriefing key moments with peers and mentors.
Preliminary Findings
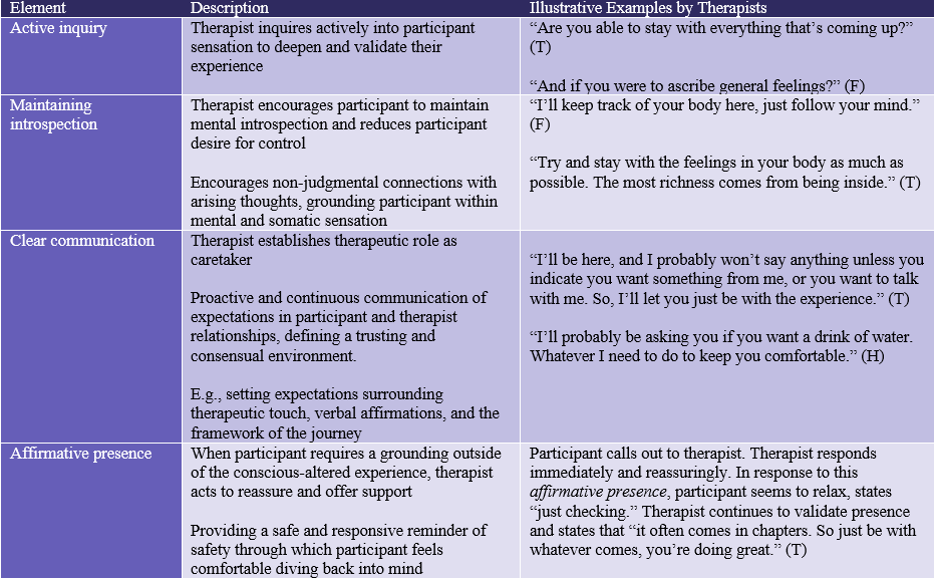
This analysis identified 4 distinct elements of interpersonal grounding: 1) active inquiry, 2) maintaining introspection, 3) clear communication, and 4) affirming presence. Each of the illustrative examples provided are pulled from different therapist and participant pairings across the four videos I analyzed. While this is not an exhaustive list of possible elements of interpersonal grounding within the context of PAT, these elements may nevertheless provide a foundation for ongoing analysis of effective forms of interpersonal grounding within participant and therapist relationships.
Interpretation of Findings
The element of active inquiry prompts active engagement between the therapist and participant, and allows both parties to situate themselves more deeply into the mental and physical sensations involved in PAT. The deeper inquiry into the journey of the participant has potential to deepen their experience and foster a more easeful healing environment.
In cases where the mind may drift from internal experience during PAT, the therapist maintaining introspection allows the participant to engage more fully in their psychedelic experience. This element emphasizes guiding the mind of the participant away from distractions or the outside world, into a deeper, more involved mental journey in which healing may occur.
Due to potential cognitive disruption and influx of emotion during PAT, therapeutic care may encompass physical as well as mental comfort. Particularly in the case of therapeutic touch and validation, clear communication is helpful to establish boundaries and appropriate modes of physical and mental comfort. This element may span communication of boundaries between therapeutic parties, to expectations of the journey itself. Clear communication emphasizes the creation of a trusting and safe environment for both parties.
In moments where PAT may incite overwhelm, affirmative presence may be used to ground participants in the physical world momentarily. When this element is practiced by a therapist, it may allow the mind of the participant a moment of reprieve from internal experience. Affirmative presence is sometimes necessary, especially if negative emotions arise during dosing, and ways of effectively practicing affirmative presence may be discussed via components involved in clear communication.
Discussion
PAT offers a promising treatment to people diagnosed with cancer who are experiencing existential suffering. Interpersonal grounding has emerged as a foundational competency within this context. Previous studies have identified that deeper focus on quality of therapeutic relationship may have an enduring impact on the therapeutic effects of PAT, with strength of relationship predicting greater emotional-breakthrough and mystical-type experience (Murphy et al., 2022). In an interview with Integrative Psychiatric Institute, Bill Richards describes interpersonal grounding “Like grounding in the electric circuit. And when you’re grounded in a good relationship, your mind can open up and work with things and go through things that it can’t do if you’re just trying to turn the biochemical soup in your brain,” (Richards, 2020). The findings in this study, identifying preliminary salient elements within PAT interpersonal grounding, may establish a foundation for future inquiry into mechanisms of developing a therapeutic relationship in this context, with potential implications for efficacy of this therapeutic practice.
References
Agrawal, M., Richards, W., Beaussant, Y., Shnayder, S., Ameli, R., Roddy, K., Stevens, N., Richards, B., Schor, N., Honstein, H., Jenkins, B., Bates, M., & Thambi, P. (2024). Psilocybin-assisted group therapy in patients with cancer diagnosed with a major depressive disorder. Cancer, 130(7), 1137–1146. https://doi.org/10.1002/cncr.35010
Association for Behavioral and Cognitive Therapies. (2023). Psychedelic-assisted therapy. ABCT. https://www.abct.org/fact-sheets/psychedelic-assisted-therapy/.
Falcon, J. 2025. “Anthropology of Psychedelics.” Anthropology of Consciousness 36: 2.
Gramling, R., Bennett, E., Curtis, K., Richards, W., Rizzo, D. M., Arnoldy, F., Hegg, L., Porter, J., Honstein, H., Pratt, S., Tarbi, E., Reblin, M., Thambi, P., & Agrawal, M. (2023). Developing a direct observation measure of therapeutic connection in psilocybin-assisted therapy: A feasibility study. Journal of Palliative Medicine. https://doi.org/10.1089/jpm.2023.0189
Garcia-Romeu, A., & Richards, W. A. (2018). Current perspectives on psychedelic therapy: use of serotonergic hallucinogens in clinical interventions. International review of psychiatry (Abingdon, England), 30(4), 291–316. https://doi.org/10.1080/09540261.2018.1486289
Griffiths, R. R., Johnson, M. W., Carducci, M. A., Umbricht, A., Richards, W. A., Richards, B. D., Cosimano, M. P., & Klinedinst, M. A. (2016). Psilocybin produces substantial and sustained decreases in depression and anxiety in patients with life-threatening cancer: A randomized double-blind trial. Journal of psychopharmacology (Oxford, England), 30(12), 1181–1197. https://doi.org/10.1177/0269881116675513
Grob, C. S., Danforth, A. L., Chopra, G. S., Hagerty, M., McKay, C. R., Halberstadt, A. L., & Greer, G. R. (2011). Pilot study of psilocybin treatment for anxiety in patients with advanced-stage cancer. Archives of general psychiatry, 68(1), 71–78. https://doi.org/10.1001/archgenpsychiatry.2010.116
Murphy, R., Kettner, H., Zeifman, R., Giribaldi, B., Kartner, L., Martell, J., … & Carhart-Harris, R. (2022). Therapeutic alliance and rapport modulate responses to psilocybin assisted therapy for depression. Frontiers in pharmacology, 12, 788155. https://www.frontiersin.org/journals/pharmacology/articles/10.3389/fphar.2021.788155/ful
Phelps J. Developing Guidelines and Competencies for the Training of Psychedelic Therapists. Journal of Humanistic Psychology. 2017, Vol. 57 (5) 450-487.
Richards, W. A., Rhead, J. C., Dileo, F. B., Yensen, R., & Kurland, A. A. (1977). The Peak Experience Variable in DPT-Assisted Psychotherapy with Cancer Patients. Journal of Psychedelic Drugs, 9(1), 1–10. https://doi.org/10.1080/02791072.1977.10472020
Richards, W. A. (2015). Sacred knowledge: Psychedelics and religious experiences. Columbia University Press.
Richards, B. (2020, August 20). Learning About Psychedelics from One of the First Pioneers – Dr. Bill Richard (K. Kurlander & W. Van Derveer, Interviewers) [Review of Learning About Psychedelics from One of the First Pioneers – Dr. Bill Richard]. In Integrative Psychiatry Institute. https://psychiatryinstitute.com/podcast/about-psychedelics-pioneers-richards/
Rodríguez Arce, J. M., & Winkelman, M. J. (2021). Psychedelics, Sociality, and Human Evolution. Frontiers in psychology, 12, 729425. https://doi.org/10.3389/fpsyg.2021.729425
Schenberg, E. E., & Gerber, K. (2022). Overcoming epistemic injustices in the biomedical study of ayahuasca: Towards ethical and sustainable regulation. Transcultural psychiatry, 59(5), 610–624. https://doi.org/10.1177/13634615211062962
Schipper, S., Nigam, K., Schmid, Y., Piechotta, V., Ljuslin, M., Beaussant, Y., … & Boehlke, C. (2024). Psychedelic‐assisted therapy for treating anxiety, depression, and existential distress in people with life‐threatening diseases. Cochrane Database of Systematic Reviews, (9). https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD015383.pub2/pdf/full
Timmermann, C., Watts, R., & Dupuis, D. (2022). Towards psychedelic apprenticeship: Developing a gentle touch for the mediation and validation of psychedelic-induced insights and revelations. Transcultural psychiatry, 59(5), 691–704. https://doi.org/10.1177/13634615221082796